Understanding ICD-10 Code R63.4 for Abnormal Weight Loss
ICD-10 weight loss code R63.4 is the clinical designation for abnormal, unintentional weight loss—specifically when the drop in body weight is significant but the underlying cause hasn’t yet been identified. It functions as a symptom code, signaling to care teams and payers alike that further investigation is needed. Critically, it’s distinct from codes tied to known diagnoses like cancer or malnutrition. Correct use of the icd-10 weight loss code R63.4 supports appropriate follow-up and helps prevent claim denials.
Clinicians should apply R63.4 only when the weight loss is both clinically meaningful and clearly unintentional—typically a notable reduction in body weight over several months that isn’t the result of a deliberate diet change or medical procedure. When unintentional weight loss stems from a documented condition, like cachexia in advanced cancer, the underlying disease code takes precedence. Either way, thorough documentation is essential to justify R63.4 and avoid coding queries down the line.
For patients and families navigating medically monitored weight changes, understanding nutrition basics can make a real difference during the evaluation period. Our guide on healthy meals for weight loss offers practical, balanced meal ideas aligned with safe nutrition principles while further workup is ongoing.
What is the ICD-10 code for weight loss?
The ICD-10 code for abnormal, unintentional weight loss is R63.4. It’s a symptom code applied when the root cause hasn’t yet been determined, and it requires supporting documentation confirming the weight loss is both significant and unintended.
Clinical Evaluation and Safety Red Flags for Unexplained Weight Loss
Unexplained weight loss demands attention—especially when it fits certain high-risk patterns. A substantial decrease in body mass over a short period is considered a serious threshold. Add symptoms like difficulty swallowing, new neurological deficits, palpable masses, swollen lymph nodes, or persistent fever and night sweats, and urgent evaluation becomes non-negotiable. These red flags can point to malignancies, chronic infections, or neurodegenerative disease Source: NCBI.
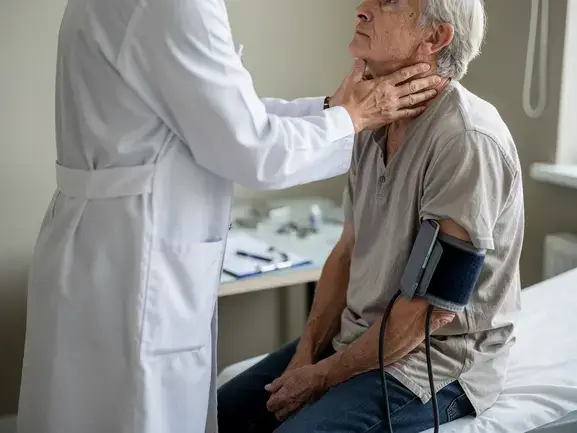
The initial workup for unexplained weight loss (ICD-10 R63.4) starts with a thorough history. Clinicians should assess how quickly the weight loss has progressed, note any systemic symptoms, and screen for changes in mental status. Medication review matters here—drugs like metformin, SSRIs, and levothyroxine can all influence body weight. A dietary review and psychosocial screening for depression or food insecurity round out the picture Source: National Cancer Institute.
Even before pinning down a cause, clinicians need to stay ahead of potential complications. Ongoing unintentional weight loss can accelerate muscle wasting (sarcopenia), weaken immune function, reduce functional capacity, and create micronutrient deficiencies—particularly in thiamine, vitamin D, and zinc. Nutritional assessment and laboratory monitoring should run in parallel with the diagnostic workup Source: PMC.
For additional support during this period, our resource on healthy meals for weight loss provides practical meal ideas that help maintain nutritional intake while evaluation is underway.
Differential Diagnosis and Recommended Workup for Weight Loss
A systematic approach to unintentional weight loss means casting a wide net early, then narrowing based on findings. Grouping potential causes into clinical categories keeps the process organized. Metabolic and endocrine disorders—hyperthyroidism, poorly controlled diabetes, adrenal insufficiency, and the rarer pheochromocytoma—top the list of medical causes. Gastrointestinal contributors include malabsorption conditions like celiac disease and chronic pancreatitis, as well as inflammatory bowel disease and chronic mesenteric ischemia. Mental health factors, particularly major depression, anxiety, and late-onset psychosis, are frequently overlooked culprits, especially in older adults (Source: American Family Physician).
Neoplastic causes should stay high on the differential—solid tumors of the lung, pancreas, stomach, and colon, along with hematologic malignancies, can all present with progressive weight loss. Chronic infections like tuberculosis, HIV, and subacute bacterial endocarditis are also worth considering when epidemiological risk factors are present (Source: NCBI).
The first-tier diagnostic workup for icd-10 weight loss (R63.4) typically includes:
- Complete blood count and comprehensive metabolic panel
- Thyroid-stimulating hormone and HbA1c
- C-reactive protein, albumin, and prealbumin
- HIV screen
- Age-appropriate cancer screenings (mammography, colonoscopy, or low-dose CT for high-risk individuals)
If first-tier results remain inconclusive and weight loss continues, second-tier investigations may be warranted. These can include chest and abdominal CT, upper and lower endoscopy, tissue transglutaminase IgA for celiac disease, and serum protein electrophoresis (Source: Merck Manual).
When initial findings are ambiguous but clinical concern persists, specialist referrals—gastroenterology, endocrinology, or psychiatry—are a reasonable next step. This structured, stepwise approach maximizes the chance of finding treatable pathology without unnecessary over-testing.
What is the ICD-10 code for R63.8?
R63.8 covers “Other symptoms and signs concerning food and fluid intake”—things like excessive appetite or feeding difficulties. It’s a separate code from R63.4 and isn’t a stand-in for it. Use R63.8 only when the symptom aligns specifically with its description.
Navigating ICD-10 Code Updates and Authoritative Sources
ICD-10-CM codes, including those related to icd-10 weight loss, are updated on an annual cycle in the United States, with changes taking effect every October 1st. The CDC and CMS jointly manage this process Source: CDC. While the WHO maintains the global ICD-10 standard, the U.S. adapted version—ICD-10-CM—includes modifications tailored to domestic clinical and billing needs.
To confirm that a code like R63.4 is still active and correctly defined, clinicians and medical coders should go directly to official resources: the CDC’s ICD-10-CM browser or the CMS website. Both publish the most current code sets and fiscal year updates Source: CMS. Commercial coding tools and unofficial summaries can lag behind or carry inaccuracies—use them cautiously.
When researching icd-10 weight loss coding guidance, prioritize documents from government agencies and professional organizations like the American Academy of Family Physicians (AAFP) or the American Health Information Management Association (AHIMA). If a site is heavily branded toward a billing vendor, cross-reference its claims with primary CDC or CMS sources before acting on them.
Staying accurate also means reviewing periodic “Coding Clinic” updates, which address ambiguous scenarios and serve as a recognized clarification authority across the country Source: CDC. Sticking to these primary sources keeps your documentation compliant, your billing accurate, and—most importantly—your patients’ records reliable.
Sources
- CDC – ICD-10-CM
- CDC – ICD-10-CM Guidelines FY2024
- NCBI – Unexplained Weight Loss Red Flags
- National Cancer Institute – Signs and Symptoms
- PMC – Nutrition Risk in Weight Loss
- American Family Physician – Unintentional Weight Loss
- NCBI – Clinical Approach to Unintentional Weight Loss
- Merck Manual – Unintentional Weight Loss
- CMS – ICD-10-CM Current Updates

